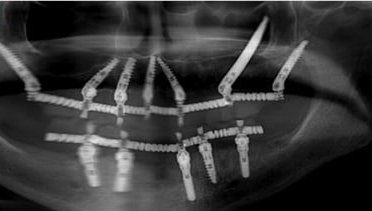
Dental Implantation has been in use for about 50 years. During this period of time, many technological and biological developments that contributed significantly to the high success rate of implantations, have taken place.
Measureable quantitative and qualitative criteria for determining the success rate of dental implants have been set by various researchers such as Alberktson and others.
The use of dental implants as part of routine dental care is growing. However, with the number of implants installed, we observe a marked increase in failure rates as well as in the incidence of pathological processes such as mucositis and perioimplantitis.
Long-term follow-ups and vast accumulated knowledge reveal a less optimistic picture of dental implantation, and the illusion that dental implants can serve as long term substitutes for natural teeth is beginning to dissipate.
Nowadays we see more and more implants losing their bony support, and aside of functional failures there is also deterioration in the uncompromised aesthetic aspect.
Therefore, more and more often clinicians are faced with the need for an upfront treatment planning of complicated cases which involve the removal of previously installed failed implants.
Having to deal with failures raises questions about the key rules in planning of implantation procedures, for example:
As it is well known, 16 mm or even 13 mm Long implants, show stability even after losing half of their support. However, once their support has been compromised, a non-reversible damage is being caused which makes their replacement,
in case of failure, much more difficult. Based on this premise, the question that comes forth is whether to choose long implants or short implants to start with.
When we offer a treatment plan to a patient who had previously installed implants that failed, we should take into consideration the etiological factors that led to this failure. It is also important to understand that the use of implants is not a lifetime solution, and therefore the planning has to take into consideration future needs of the patient.
The following case presents a 64 years old female patient
The clinical examination showed:
- Chronic generalized severe periodontitis;
- Peri-Implantitis and Mucositis around implant’s in the lower jaw;
- Calculus and plaque accumulation;
- Implants’ threads exposure;
- Bleeding on probing;
- Periodontal pockets and mobility;
- Secondary caries in some of the restorations;
- Periapical lesions associated with the right mandibular premolars;
Treatment plan:
- Clearance – Extractions of all teeth and implants (mandible and maxilla);
- Installation of 7 implants in maxilla, out of which
- 2 Tubero Pterygoid Palatine implants (TPP)
- 1 Zygoma implant by extra maxillary approach;
- 2 tilted implants (the right one being parallel to the sinus mesial wall);
- 2 parallel implants at the anterior region;
- Lower jaw- 5 implants, out of which 4 in the intremental region. 4 of which are Cortical type implants;
Lower Jaw
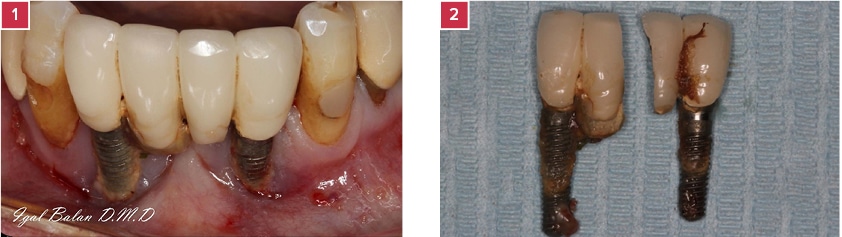
- Clinical image of the lower jaw prior to the extraction. Calculus and Plaque accumulation, Implant Threads exposure, Peri-Implantitis, and Mucositis are observed.
- Old Implants post extraction.
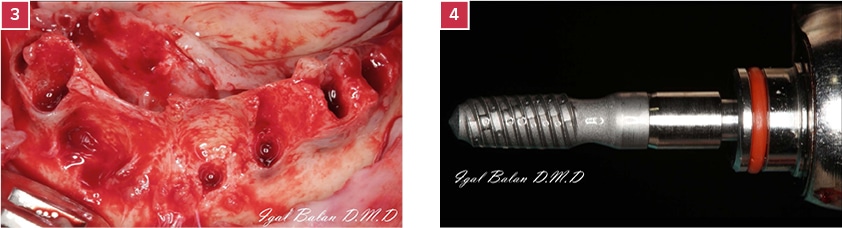
3. Lower jaw after the extractions. Extensive bony defects at the extraction sites are observed.
4. A Cortical implant with aggressive threads, designed to provide excellent primary stability.
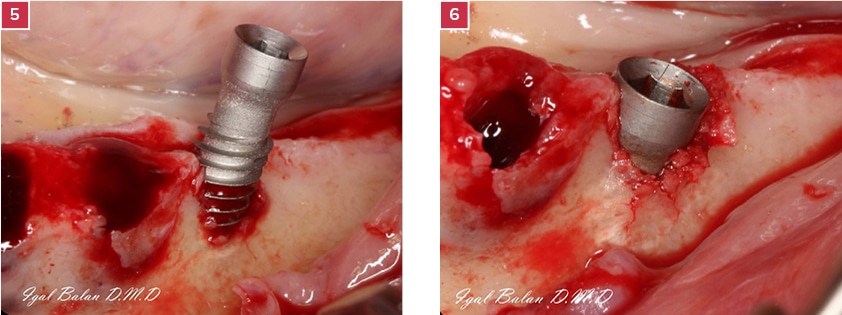
5. Cortical implant inserted at the extraction site.
6. The neck of the implant remains exposed. The smooth neck minimizes the adherence of periopathogens.
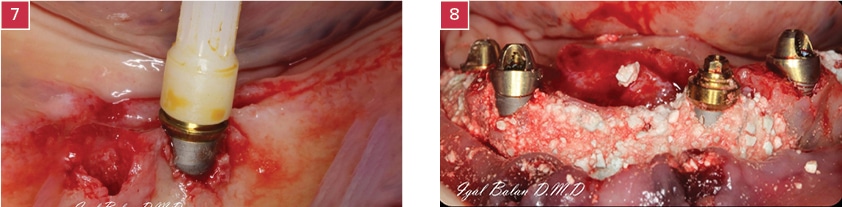
7. A Multi-Unit abutment is mounted on the implant.
8. Bone augmentation using HA & Calcium sulfate bone graft
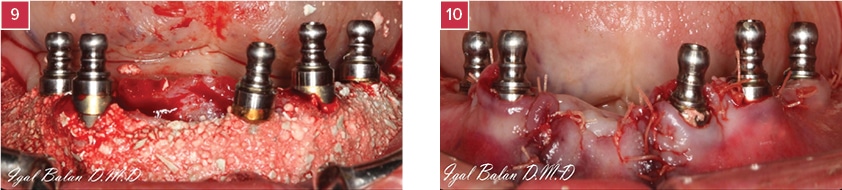
9. Snap-On Transfer bases are mounted on the Multi-Unit.
10. Suturing around the transfer bases
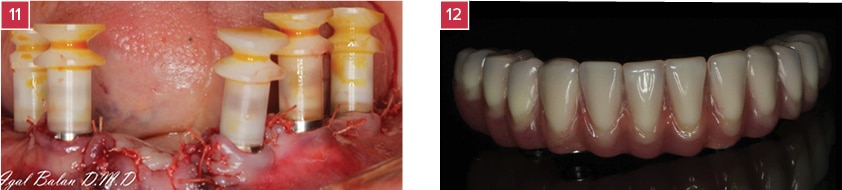
11. The female components of the transfers are being mounted on the male components.
12. Reinforced provisional lower acrylic bridge.
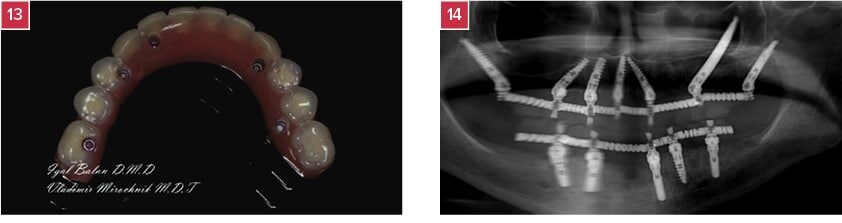
13. Occlusal view of the lower acrylic bridge.
14. Panoramic X-Ray (with the provisional bridge) at the end of the operation.